Irina Alexandrovna Zborovskaya – doctor of medical sciences, professor, head of the department of hospital therapy with the course of clinical rheumatology of the doctors improvement faculty of Volgograd state medical university, deputy director for scientific work of the State institution “Research and development institute of clinical and experimental rheumatology” of the RAMS, head of the regional Osteoporosis Center, presidium member of the Association of rheumatologists of Russia, member of the editorial boards of the magazines “Scientific and practical rheumatology” and “Modern rheumatology”
Definition. Rheumatoid arthritis (RA) refers to a chronic systemic inflammatory disease of the connective tissue which is commonly characterised by progressing erosive-destructive polyarthritis, rapid development of functional changes in the affected joints and certain extraarticular manifestations.
Epidemiology. The prevalence of RA among adults is about 1%. Clinical forms of RA are observed in 0.5% of women and 0.1% of men. Females are 3 times more likely to develop RA than males. The frequency of RA increases with age and the disease is observed both in females and males with similar prevalence rates. Rheumatoid arthritis affects all populations worldwide.
Aetiology. Nowadays no organism has been proven responsible for RA.
Infectious factors. The revealing of virus-like particles in the synovial membrane at the early stage of the disease as well as the development of polyarthritis in some viral and infectious diseases has proven an infectious aetiology of RA. The following infectious agents have been suggested to induce RA:
Streptoccocus B,
Mycoplasma organisms, Epstein-Barr and rubella viruses. The frequency of getting lymphocytes infected with Epstein-Barr viruses increases in patients with RA compared to healthy people. Antibodies to Epstein-Barr viruses are present in 80% of patients with RA.
As no infectious agent has been found responsible for RA, the infectious atiology of RA has not been proven yet.
Genetic factors. First-degree relatives of patients with RA have an increased frequency of disease which is 4 times more than the prevalence of RA among the population. Kinsmen (relatives by blood) are 16 times more likely to develop RA. Approximately 10% of patients with RA have first-degree relatives suffering from RA. Disease concordance in monozygotic twins is 4 times more than in dizygotic twins or in siblings which is approximately 15 – 20%, suggesting that not only genetic factors play an important role in pathogenesis of the disease.
It has been established that HLA-Dw4 (DRB1*0401) or НLА-Dw14 (DRB1*0404) carriers have the risk of developing RA 1: 35 (one to thirty-five) and 1:20 (one to twenty), respectively. The risk of developing the disease is more higher in carriers of both types. At the same time НLА-DR5, НLА-DR2, НLА-DR3 and НLА-DR7 clusters may prevent the person from developing RA, as the clusters are less commonly revealed in patients with RA than in healthy people.
Hormonal factors. Sex hormones and prolactin may play a role, as evidenced by disproportionate number of females with RA under 50 (females are 2 – 3 times more likely to develop RA than males but with age the disease is observed in females and males with similar prevalence rates).
Reduced incidence of RA during pregnancy and in women using oral contraceptives has also been reported.
Pathogenesis. RA is associated with a number of autoimmune abnormalities as well as with imbalance of quantitative and qualitative composition of immunocompetent cells and impaired functional activity of cells and cellular cooperation. Th 1 cells are supposed to play a major role in the initiation of RA and they are the main producers of proinflammatory cytokines which are produced in excessive amounts in RA.
It is suggested that at the early stage of RA joints are affected due to a nonspecific inflammatory reaction induced by different stimuli resulting in destruction of synovial cells in genetically predisposed people. As a result of the involvement of the immune cells in the articular cavity, an “ectopic” lymphoid organ is formed whose cells begin to synthesize autoantibodies to the components of the synovial membrane.
T-lymphocytes CD4+ and CD8+ prevail in cellular infiltrates in the synovial membrane. In addition to T-lymphocytes, there are many B-lymphocytes in it. Activated CD4-lymphocytes stimulate proliferation of B-lymphocytes and their arrival into plasma cells which secrete autoantibodies, including rheumatoid factor (RF). Fibroblasts become activated and begin to produce proteolytic enzymes. The number of osteoclasts increases in the areas of bone destruction.
Activated cells of the synovial membrane produce great amounts of cytokines, such as TNF-alfa, interleukines 1, 2, 6, 8, 10, growth factors, interferons. These cytokines stimulate the inflammatory reaction, the arrival of cells and mediators of inflammation into the synovial fluid, proliferation of synoviocytes. They participate in cartilage and bone destruction as well as in the development of
extraarticular manifestations of RA. Histamine and other vasoactive substances produced by mast cells of the synovial membrane stimulate migration of neutrophils and other cells into the synovial fluid. Finally, prostaglandin E2 which is produced in the synovial membrane has a vasodilatory action and contributes to the arrival of cells into the area of inflammation.
It should be noted that progression of RA is a dynamic process which is divided into 3 stages:
- Early (asymptomatic) stage of RA. It is characterized by vascular and cellular activation.
- Extensive stage of RA (progressing chronization of inflammation). It is characterized by impaired angiogenesis, activation of endothelium, cellular migration, infiltration of the synovial tissue by CD4+T-lymphocytes, serum RF (rheumatoid factor) and immune complexes, synthesis of proinflammatory cytokines, prostaglandins, collagenase, metalloproteinase.
- Advanced stage of RA which is characterized by somatic mutation and defects of apoptosis of synovial cells.
Pathomorphology. Morphologic processes of disorganization of the connective tissue occur mainly in joints. Synovitis is manifested clinically by various combinations of exudative-alterative and proliferative processes. It is often characterized by lymphoid infiltration of the synovial membrane, vasculitis with resultant perivascular infiltration, mucoid swelling and sclerosis of the synovial membrane.
Formation of new vessels which is characterized by transudation and transmigration of lymphocytes into the synovial tissue and leukocytes into the synovial fluid is a typical early finding of rheumatoid synovitis.
Lymphoid infiltration of the synovial membrane has a peculiar structure of rheumatoid granuloma in which fibrin is surrounded by mesenchimal cells on the surface of the synovial membrane covered by lymphoid cells.
Formation of an ectopic focus of hyperplasia of the synovial tissue is considered to be the most significant morphological characteristics of rheumatoid inflammation. Its invasive growth (pannus) often results in the destruction of the articular cartilage and subchondral bone.
Loose granulation tissue (pannus) destroys the cartilage and epiphyses of bones resulting in erosive arthritis.
Stages of joint involvement:
I stage – hypertrophy of the synovial membrane;
II stage – proliferation of pannus into the meniscus;
III stage – focal destruction of the meniscus;
IV – complete destruction of the meniscus and focal destruction of the articular surface;
V stage – fibrous ankylosis resulting in bony ankylosis.
Rheumatoid nodule is a specific histologic feature of RA and is considered to be a focus of fibrinoid necrosis surrounded by macrophages, lymphocytes and plasmocytes.
Rheumatoid nodules may be present in the synovial membrane, tendon sheaths and they may be accumulated in the periarticular subcutaneous fatty tissue.
Morphological substrates of extraarticular involvement in RA are considered to be vasculitis and rheumatoid granulema found in internal organs.
Clinical manifestations. In two-thirds of patients the disease progresses slowly and is clinically characterised by systemic features, such as malaise, loss of appetite, weakness and involvement of the musculoskeletal system before the appearance of overt joint inflammation and swelling. As the disease progresses, the patient develops common symptoms of RA, such as symmetric arthritis with involvement of hand, knee, ankle, and wrist joints.
Joint involvement. Bilateral symmetric involvement of joints (except distal interphalangeal joints) is common in patients with RA. Small joints of the hands and feet are commonly affected. Those most commonly affected joints are the second and third metacarpophalangeal joints, proximal interphalangeal joints, the second and fifth metatarsophalangeal joints. Morning stiffness which occurs after a long period of rest is the characteristic feature of RA. The involved joints are usually painful when palpated and have a paste-like consistency. Their contours are smoothed and the joints are increased in size due to exudation, hypertrophy of the synovial membrane and thickening of the articular capsule.
The temperature of the skin around joints is increased. The affected joints show decreased range of motion. Most patients have muscle atrophy, which is secondary to joint inflammation.
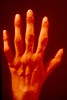
“Rheumatoid hand” refers to a swelling of the wrist, metacarpophalangeal joints and atrophy of interosseous muscles.
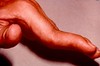
Most patients develop articular deviations due to the formation of an angle between two adjacent bones. When fingers are inclined to the ulna, the patient develops ulnar deviation due to the destruction of the heads of metacarpal bones and weakness of muscles. The hand looks like a sean-fin. Flexion deformities in metacarpophalangeal joints, hyperextension of proximal interphalangeal joints and flexion of distal joints of fingers may lead to swan-neck deformities.
Excessive flexion of metacarpophalangeal joints, proximal interphalangeal joints and hyperextension of distal interphalangeal joints may lead to bouton deformities. Shortening of the phalanges with ulnar deviation may lead to deformities such as “a hand with a lorgnette”.
Inflammatory involvement of the
elbow may lead to limited movements of the joint resulting in the development of deformity in the position of semiflexion and semipronation as well as entrapment of the ulnar nerve and paresthesia of the nerve supply area. The most common clinical manifestations of
shoulder involvement are swollen, painful joints when palpated or in active or passive movements as well as impaired mobility of the joint resulting in the atrophy of the interosseous muscles.
Hip joint is less commonly affected in RA. When hip is involved, the patient has pain spreading to the inguinal or inferior parts of the gluteal region. Limited movements of the internal rotation of the low extremity is another commonly observed manifestation.
Fixation of the hip in the position of semiflexion is a typical finding.
Involvement of
knee joints is characterized by their swelling due to synovitis and tenderness in performing active and passive movements. Due to high intraarticular pressure the posterior part of the articular bursa is often herniated into the popliteal space forming Baker`s cyst.
Most commonly affected
joints of foot are the second and forth metatarsophalangeal joints. Joint involvement may lead to its defiguration and deformity of foot due to multiple subluxations and joint ankylosis.
Joint involvement may also lead to hallux valgus, subluxation of the heads of metatarsal bones resulting in their displacement to the side of the sole, widening of the anterior part of the foot, hallux valgus, subluxation of toes and their displacement upwards and towards the lateral side of the sole.
Ankle involvement is manifested clinically by pain and swelling around the ankle. Inflammation of the synovial membrane of ligaments and tendons is the characteristic feature of patients with RA.
Cervical spine is frequently affected. Arthritis of intravertebral joints of the upper cervical vertebrae may lead to atlantoaxial subluxation. Symptoms include pain spreading to the occiput, spinal cord compression and compression of the vertebral artery.
Extraarticular (systemic) manifestations.
Rheumatoid nodules are referred to as the most widespread extraarticular features of RA and they may be present in 20 – 30% of patients. They are localized in the area of the elbow, Achilles tendon, on the extensor surface of the forearm and in the occiput.
Rheumatoid nodules are painless and motile. However, they may be connected with aponeurosis or bone.
Skin involvement in patients with RA is manifested by impaired trophism, subcutaneous hemorrhages and piecemeal necrosis due to developing vasculitis.
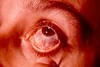
Eye involvement in patients with RA is manifested clinically by iritis, iridocyclitis, episcleritis and scleritis. Iridocyclitis is most common (3.5% of all cases) in patients with RA. Episcleritis is characterised by moderate pain, segmental reddening of the anterior part of the eye. Scleritis is characterised by severe pain, hyperemia of the sclera that may lead to loss of vision.
Effect of RA on the heart. Pericarditis characterised by pericardial effusion is common in RA. Myocarditis in patients with RA is often asymptomatic. Rheumatoid nodules can involve myocardium.
RA involvement of the lungs may take the following forms: pleuritis, chronic interstitial pneumonitis, rheumatoid nodules and pulmonary vasculitis. All these conditions are most commonly asymptomatic.
Dry (fibrinous) pleuritis is more likely to develop than interstitial pneumonitis which is the ultimate cause of death associated with lung involvement. It is manifested clinically by progressing dyspnea, crepitation (crackling) in the basal parts of the lungs, bilateral interstitial or infiltrative changes on lung radiographs.
Rheumatoid nodules are usually discovered accidentally on joint radiographs. Some patients with RA develop pulmonary vasculitis underlying immunocomplex impairment of pulmonary vessels and microcirculation.
Kidney involvement in patients with RA is observed in 10 –25% of cases. Amyloidosis is the most common causative factor of kidney involvement. It develops within 7 –10 years after the appearance of articular syndrome. Proteinuria is most common in patients with RA and is manifested by various clinical presentations. It may also cause disorders of concentration function and nitrogen-releasing function of kidneys, anemia, moderate hypertension and renal failure.
Patients with RA may also develop mesangial-proliferative or membranous glomerulonephritis which is manifested clinically as urinary syndrome. Sometimes patients with RA may develop, however, complete or incomplete nephrotic syndrome (massive proteinuria, hypo-and disproteinemia, dislipidemia) resulting in pronounced edema and arterial hypertension. Unlike amyloidosis, the prognosis of rheumatoid glomerulonephritis is favourable.
Patients with RA may have neuropathy which is the most common
impairment of the nervous system.
Three main types of neuropathy are singled out. They are the following:
- Mononeuritis multiplex which is characterized by the impairment of certain nerve trunks with corresponding motor and sensitive dysfunctions.
- Symmetric peripheric neuropathy. It may be either sensitive or motor-sensitive.
- Compression neuropathy. It includes entrapment of the median nerve in the area of the wrist (carpal tunnel syndrome), entrapment of the tibial nerve in the area of the medial malleolus (tarsal tunnel syndrome).
Vegetative nervous system disturbances are common and they are manifested by hyper- or hypothermia, increased sweating and trophic disturbances.
Rheumatoid vasculitis occurs in 8 – 20% of patients with RA. Males are more likely to develop rheumatoid vasculitis than females and it can affect any organ or system. The activity of vasculitis depends on the extent of rheumatoid inflammation and it usually complicates the course of the disease. Neuropathy is a common symptom of vasculitis.
Muscle involvement is manifested clinically by myalgia at the early stage of the disease. It is manifested by myositis with foci of necrosis and muscular atrophy at the advanced stage.
Peripheral lymphadenopathy is diagnosed in 40 – 60% of patients with RA. Anterior and posterior cervical lymph nodes, submandibular, sub- and supraclavicular lymph nodes, axillary lymph nodes and inguinal lymph nodes are most commonly affected.
Splenomegaly is observed in 25 – 30% of patients with RA.
Gastric and intestinal disturbances are reported in 50% of patients with RA and are often secondary to associated processes such as medication effects. Sometimes patients with RA develop amyloidosis of the gastrointestinal tract which is clinically manifested by malabsorption.
Autoimmune thyroiditis is common in patients with RA. The most common clinical manifestations of autoimmune thyroiditis are swollen and painful thyroid gland when palpated as well as formation of antibodies to the tissue of the thyroid gland.
Laboratory studies. No pathognomonic (specific) test is available to help confirm the diagnosis of RA.
High-titered rheumatoid factor (RF) which is an antibody to Fc-receptor of IgG (immunoglobulin) is present in approximately 80% of patients with RA. Rheumatoid factor is not, however, specific for the diagnosis of RA and it cannot be used as a screening method. Anemia of chronic disease is common and correlates with disease activity. Leukocytosis is less common but it may occur in certain joint and organ involvement, serious infections or it may be a consequence of corticosteriod therapy. Neutrophilic leukocytosis is common in patients with Still’s disease (juvenile rheumatoid arthritis). Granulocytopenia, splenomegaly and severe joint involvement may occur in patients with Felty syndrome. Elevated ESR (erythrocyte sedimentation rate) is associated with disease activity. Elevated C-reactive protein is also common in patients with RA.
Classification of Rheumatoid Arthritis
| Clinical anatomical characteristics |
Clinical immunological characteristics |
Course of the disease |
Stage of the disease activity |
Stage of the disease determined according to X-ray examination |
Functional status of the patient |
| Rheumatoid arthritis:-polyarthritis
-oligoarthritis
-monoarthritis
Systemic features of rheumatoid arthritis:
– involvement of the reticuloendothelial system, lungs, heart, nervous system; amyloidosis of organs
Specific symptoms:
– pseudoseptic syndrome
– Felty’s syndrome
Other commonly observed musculoskeletal manifestations:
– osteoarthrosis;
– diffuse diseases of the connective tissue;
– rheumatism.
Juvenile arthritis (including Still’s disease)
|
SeropositiveSeronegative |
The disease progresses rapidly
The disease progresses slowly
Without a well marked progression
|
I – slow progressionII – moderate progression
III – severe progression
IV – remission of RA |
I – paraarticular osteoporosis;II – osteoporosis, narrowing of the articular space and occasionally the patient may suffer from early bone attrition;
III – osteoporosis, narrowing of the articular space and the patient may suffer from extensive attrition of bone;
IV – osteoporosis, narrowing of the articular space and occasionally bony ankylosis.
|
0 – the patient is healthy;I – the patient is able to work and perform usual activities;
II – the patient cannot work;
III – the patient is limited in ability to perform usual self-care.
|
Clinical laboratory characteristics of rheumatoid arthritis activity
| Feature |
Activity |
| 0 |
I |
II |
III |
| Joint pain |
0 |
1 – 3 |
4 – 6 |
7 – 10 |
| Duration of morning stiffness, min |
15 – 30 |
30 – 60 |
Until noon |
All day long |
| Number of inflamed/painful joints |
0 |
Up to 3 |
4-6 |
More than 6 |
| Number of systemic signs |
0 |
Vasculitis is present |
1 – 3 |
More than 3 systemic signs or vasculitis may be present |
| Hemoglobin, g/l |
More than 130 |
129 – 120 |
119 – 110 |
Less than 109 |
| ESR, mm/hr |
More than 10 |
10 – 20 |
21 – 40 |
More than 40 |
| C-reactive protein |
Less than 1,0(0) |
1.1 – 1.5(+) |
1.6 – 2.0(++) |
More than 2(+++) |
Synovial fluid analysis is of great importance to patients with RA. The concentration of protein rises up to 40 – 70 g/l in RA, while in degenerative joint diseases it is 20 – 30 g/l (grams per litre).
Cytologic analysis of the synovial fluid enables us to evaluate the extent of the inflammatory process: in high activity of RA increased cytosis is present (up to 15 – 20*10
9/l (per litre) cells and even more). Segmental leukocyte and phagocyte predominance (more than 80% and 50% respectively) is observed in the synovial fluid. Hemolytic activity of the complement and the level of C3 and C4 components in the synovial fluid are often low.
Diagnosis. RA can be easily diagnosed at the extensive stage. In most cases, however, the most common symptoms usually appear in 1 – 2 years after the onset of the disease.
Diagnostic criteria of rheumatoid arthritis developed by the American College of Rheumatology (1987)
1. Principles of diagnostics
- To make a diagnosis of RA, at least four of the seven criteria of the American Rheumatology Association must be present.
- Additionally, there should not be evidence of other disease that may account for the symptoms of RA.
2. Criteria
- Morning stiffness. This occurs in and around the joints and lasts at least 1 hour.
- Arthritis of 3 or more joint areas. At least 3 joint areas simultaneously have soft tissue swelling or fluid. Other possible areas are proximal interphalangeal (PIP), metacarpophalangeal (MCP), wrist, elbow, knee, ankle, and metatarsophalangeal (MTP) joints.
- Arthritis of at least one area in a wrist, metacarpophalangeal (MCP) or proximal interphalangeal (PIP) joint.
- Symmetric arthritis with simultaneous involvement of the same joint areas on both sides of the body. Bilateral involvement of PIPs, MCPs, and MTPs is acceptable without absolute symmetry.
- Rheumatoid nodules. Subcutaneous nodules are present over bony prominences or extensor surfaces or in juxta-articular regions.
- Positive serum rheumatoid factor. Abnormal amounts of serum RF are demonstrated by any method for which the result has been positive in fewer than 5% of healthy control subjects.
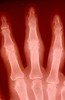
- Radiographic changes typical of RA on hand and wrist radiographs which must include erosions or osteopenia.
Criteria A-D must be present for at least 6 weeks, and the physician must observe criteria B-E.
Poor prognostic indicators of RA:
- Gradual onset of the disease;
- Early involvement of large joints;
- Persistent activity of the disease;
- Revealing of abnormal amounts of serum RF in the first year of the disease;
- High-titered RF;
- Early attrition of bone;
- Presence of HLA-DR4/D4 clusters.
Diseases which have to be differentiated from RA:
- Polyosteoarthrosis
- Gouty arthritis and pseudogout
- Ankylosing [rheumatoid] spondylitis
- Reactive arthritis and Reiter’s syndrome
- Infectious arthritis (tuberculous arthritis, Lime’s disease, gonococcal arthritis)
- Arthritis occuring in viral infections (rubella, hepatitis B, retroviral infection)
- Systemic diseases of the connective tissue (systemic lupus erythematosus, systemic scleroderma, polymyositis, dermatomyositis, rheumatoid polymyalgia, systemic vasculitis)
- Hypertrophic osteoarthropathy
- Paraneoplastic polyarthropathy
- Sarcoidosis
Treatment of RA.
Methods of treatment:
- Treatment of patients with RA should be prolonged, complex, continuous and must be individualized.
- Treatment should be aimed at relieving pain and reducing inflammation.
- The main objective of treatment is to preserve the range of motion of joints and to help patients to cope with daily life.
The most important objective of treatment is to achieve and maintain clinical and laboratory remission or clinical improvement in patients with RA. To achieve the above mentioned objectives, it is necessary to solve the following problems:
- controlling inflammation and pain syndromes by administering anti-inflammatory drugs and analgesics;
- receiving basic therapy preventing progression of the disease and effecting the main pathogenetic mechanisms of RA.
Drug (pharmacologic) therapy.
Nonsteroidal anti-inflammatory drugs (NSAID) interferes with prostaglandin synthesis and (or) leukocyte functioning, thus reducing pain and inflammation. The efficacy of different NSAID in therapeutic doses is comparable and the selection of a certain drug for the patient is performed empirically, by selecting a drug. The most common side-effect in long-term use of NSAID is “nonsteroidal anti-inflammatory gastropathy” which is manifested clinically by dyspeptic disturbances, impaired gastric and duodenal mucosa. Selective cyclooxigenase – 2 (COX-2) inhibitors, such as meloxicam, celecoxib, rofecoxib, have been widely used recently. They cause gastrointestinal disturbances less commonly than standard nonsteroidal anti-inflammatory drugs.
However, they may also have some side-effects, such as dyspepsia, poor gastrointestinal ulcer healing, fluid retention and increased blood pressure.
Glucocorticoids are potent anti-inflammatory drugs but at the same time they are highly toxic and may cause Cushing’s syndrome, adrenocortical insufficiency, gastropathy, arterial hypertension, diabetes mellitus, osteoporosis, myopathy. Besides this, long-term use of glucocorticoids in patients with RA may result in the development of various infectious complications due to susceptibility to infection.
Indications for administering glucocorticoids are the following: severe RA accompanied by visceritis, pseudoseptic syndrome. Glucocorticoids should also be administered in case of unsuccessful NSAID (nonsteroidal anti-inflammatory drug) therapy. Doses of up to 7.5 – 15 mg of prednisone are typically used; in severe RA doses of up to 30 – 60 mg are used. The dose is administered until achieving the therapeutic effect and then it is reduced every 5 – 7 days up to maintenance dose.
Intraarticular administration of glucocorticoids is prescribed as an additional measure. Hydrocortisone may be given 50 – 125 mg in large joints, 25 – 50 mg in middle-sized joints, 5 – 10 mg in small joints). Single dose of triamcinolone is 10 – 20 mg in large joints, single dose of methylprednisolone is 40 mg in large joints, and single dose of betametasone is 1ml in large joints and 0.5 ml in smaller joints. Local administration of glucocorticoids may give temporary relief.
Disease-modifying antirheumatic drugs. Disease-modifying drugs should be considered for use early in the course of RA. Selection of a disease-modifying drug must be individualized.
Aminoquinoline drugs (chloroquine, hydroxychloroquine) are administered in joint diseases and, especially when the disease progresses slowly. Aminoquinoline drugs should be used for approximately 3 – 6 months or 6 – 12 months before one decides on efficacy. The patients are quite tolerant to aminoquinoline drugs, however, they may develop some side effects, such as dyspepsia, itching, dizziness, transient leucopenia, pigmented retinitis, accumulation of the drug in the cornea.
Gold salts are effective in treating patients with RA. They are administered if there are not any systemic lesions. Mechanisms of their action have not been studied yet. Treatment should be started with single dose of 5 – 25 mg of gold salt followed by 5 – 25 mg 1 (one) week later to test for sensitivity. If the patient is tolerant to the drug, 17 – 34 mg should be administered weekly. If there is improvement with a cumulative dose of 1 or 2 g, maintenance therapy is 34 mg monthly for 1 – 2 years or sometimes it can be prolonged up to 5 – 10 years.
Drug dermatitis, nephropathy, leucopenia, thrombocytopenia, anemia, toxic hepatitis, cholestasis, pancreatitis, erosive lesions of the gastrointestinal tract, photosensitivity are common side effects.
Methotrexate is a known antagonist of folic acid. It is used in seropositive patients with active RA. The effects of the drug begin to appear in the forth and eighth weeks and reach their peak by the sixth month.
Methotrexate is effective when administered 7.5 – 25 mg weekly. Its use results in slowing down the destruction of joints.
Parenteral administration of
Methotrexate is prescribed if oral administration is unsuccessful or if toxicity develops.
Serious side effects are gastrointestinal disturbances, oral mucosa ulcers and disorders of hepatic function. These side effects are reversible when the drug is discontinued.
Sulphasalazine slows down the destruction of joints reducing inflammation. It is relatively safe and effective in patients of all age groups irrespectively of the duration of the disease and presence of RF. It can be used in combination with other drugs. The initial dose should be 1 g daily and then increasing doses to 2 – 3 g daily for maintenance.
Sulphasalazine should be used for approximately 3 months or 8 – 12 months before one decides on efficacy.
Leflunomid is a new basic antirheumatic drug developed particularly for treating RA.
Leflunomid has immunomodulating activity and reduces inflammation. The initial dose of
Leflunomid 10 – 25 mg daily has been shown to improve the patient’s condition.
Leflunomid is as efficient and safe as methotrexate. Serious adverse reactions include hepatic diseases, immunodeficiency. Concomitant
Rimphampycine increases
Leflunomid concentration.
D-penicillinamine is used in progressive destruction of joints. It is contraindicated in articular-visceral forms of RA, renal, pulmonary diseases, active hepatitis and liver cirrhosis. Doses must be individualized and they are variable.
Cyclosporine A is recommended to the patients with RA who are unresponsive to other drugs. The use of
Cyclosporine A helps to improve the patient’s condition, however, it results in the involvement of the gastrointestinal tract and kidneys. The initial dose is 1.5 – 3 mg/kg daily and then it is necessary to increase the dose to the optimum one depending on efficacy and patient’s tolerance of the drug.
Cyclosporine A should be used for approximately 6 – 12 weeks before one decides on efficacy. The maximum dose must not exceed 5 m/kg daily.
Cytostatics (azathioprine and cyclophosphamide) are administered in severe articular-visceral forms of RA, including “malignant” and “pseudoseptic” joint involvement which are characterised by high activity and a torpid course of the disease as well as if conticosteroid therapy was unsuccessful. Cytostatics have a well pronounced immunosuppressive action providing adequate control over the course of the disease. Immunosuppressive therapy, however, often involves some side-effects. These side-effects include changes of peripheral blood composition (leuko- and thrombocytopenia, agranulocytosis), decreased resistance of the body to infectious agents which may lead to the development of pneumonia,
Herpes zoster, pyoderma, aggravation in the foci of chronic infection and others.
Since
Azathioprine or
Cyclophosphamide therapy doesn’t always enable us to control the progression of RA, the questions of concomitant therapy with other drugs are being studied now. Combinations of
Cyclosporine and
Methotrexate as well as
Methotrexate,
Sulphasalazine and
Hydroxylchloroquine have been well studied.
One of the most important achievements of pharmacotherapy of RA is associated with the development of a new group of drugs called
biological agents or anticytokine therapy.
Infliximab,
Adalimumab referred as monoclonal antibodies against TNF-alpha; recombinant soluble receptor TNF-alfa,
Etanercept linked to the Fc portion of human IgG; and, recombinant soluble antagonist IL-1 –
Anakinra are used nowadays for treating RA.
These drugs are effective both in combination with
Methotrexate in patients with active RA who are unresponsive to
Methotrexate and when used separately.
In Russia
Infliximab is allowed for the treatment RA. It is very useful resulting in rapid positive dynamics. It slows down the destruction of joints irrespectively of sex and age of the patient. The main indication for administering
Infliximab is persistent RA despite the use of
Methotrexate.
Apheresis procedures are being investigated now. These methods are supposed to be useful due to their immunocorrective, rheocorrecting and detoxication effects.
The indications for apheresis procedures are the following: systemic lesions, persistent inflammation, rapid progression of the disease, ineffectiveness of drug therapy. Apheresis procedures include
plasmapheresis (that is removal of plasma),
lymphocytopheresis (that is removal of lymphocytes),
cascade filtration of plasma,
immunosorption, cryoplasmosorption, hemosorption,
photochemotherapy.
Surgical treatment. Early surgery of RA includes such operations as
synovectomy, tendonsynovectomy. Inflammation of joints in most patients undergoing operative treatment is controlled. The most effective is considered to be early synovectomy of knee and elbow joints.
Reconstructive and restorative operations are often undertaken at the advanced stage of the disease. These operations include
extensive synovcapsulectomy (debridement), arthroplasty and endoprosthesis.
In flexion contractures remedial procedures, such as
capsulotomy, osteotomy are performed.
Arthrodesis, i.e. (that is) a complete closure of the joint in the physiologically favourable position results in complete and constant controlling of arthritis in the operated joint. However, the motor function of the joint is lost.
Prognosis. The prognosis depends on the activity of the disease. Approximately 50% of patients will not be working after 3 years. In most cases long-term prognosis is rather favourable. However, in case of visceritis, long-term prognosis is worse.