Просмотров: 8 961
Osteoarthrosis (OA)
Irina Alexandrovna Zborovskaya – doctor of medical sciences, professor,cathedral professor of hospital therapy with the course of clinical rheumatology of the doctors improvement faculty of Volgograd state medical university, director of the Federal Budgetary State Institution (FBSI) “Research and development institute of clinical and experimental rheumatology” of the RAMS, head of the regional Osteoporosis Center, presidium member of the Association of rheumatologists of Russia, member of the editorial boards of the magazines “Scientific and practical rheumatology” and “Modern rheumatology”
Definition. Osteoarthrosis is a chronic progressive degenerative-dystrophic disease of joints characterized by degeneration of the articular cartilage, changes in the subchondral bone and hypertrophy of bone at the margins. It is often associated with acute or latent synovitis.
Epidemiology. Females are 2 times more likely to develop osteoarthrosis than males. The incidence of joint involvement does not depend on sex in people under 55. The hip is most commonly affected in men over 55; knee joint, carpometacarpal joints and distal interphalangeal joints are typically affected in women. The symptoms of osteoarthrosis are observed in 2% of women under 15 years, in 30% of women from 45 till 64 years and in 68% of women over 65 years.
Different prevalences of osteoarthrosis and localization of the lesion have been cited for different ethnic groups. Family incidence is 2 times more than the population incidence. The risk of developing osteoarthrosis is 7.7 times higher in people with congenital defects of the musculoskeletal system.
Aetiology. Oteoarthrosis is a multi – factorial disease. However, there are two main factors underlying the onset of the disease and the extent of joint involvement. They are the following: the articular cartilage is under constant mechanical and emotional stresses, that is why its resistance to ordinary physiologic load is reduced.
1. Traumatism. Trauma and stereotype movements are the main risk factors for getting osteoarthrosis. Joint involvement may occur either at the moment of trauma or later in life (for example, when moving a joint). Sportsmen and people of the related professions may develop osteoarthrosis of joints which are not commonly affected. Thus, ballet-dancers often develop osteoarthrosis of the ankle, ballplayers most commonly develop osteoarthrosis of the elbow and boxers most commonly have osteoarthrosis of metacarpophalangeal joints.
Small chronic traumas of the articular surface of cartilage contributes to the reduction of its ability to resist mechanical load resulting in degeneration of cartilage tissue.
2. Various operations (for example, meniscectomy, etc.), acquired diseases of bones and joints.
3. Age peculiarities. Aging is associated with the following changes:
1) Decreased proteoglycan aggregation.
2) Estrogen deficiency (in postmenopausal women).
3) Loosening of collagen II type
4. Genetic factors.
a) Females are 10 times more likely to develop erosive osteoarthrosis than males. It is accounted for by the fact that autosome-dominant characteristics are more likely to be inherited by females, while recessive characteristics are typically inherited by males.
b) Collagen type II defects. Examples include Stickler arthro-ophthalmopathy syndrome which is considered as a complex of congenital developmental abnormalities of joints and eyes. It is typically referred to as polyarticular osteoarthrosis which most commonly affects young adults.
5. Inflammation
6. Obesity is considered to be a risk factor for getting osteoarthrosis of knee and carpal joints. Reduction of body weight by 5 kg decreases the risk of osteoarthrosis of knee joints.
7. Neuropathy. Impaired proprioceptive impulses contribute to the reduction of muscular tone, gradual increase of physical load on the joint resulting in osteoarthrosis.
8. Some substances can accumulate in the cartilage matrix resulting in affection of chondrocytes and restriction of joint movement.
Pathogenesis. The processes of synthesis and degeneration in the articular cartilage are well balanced. Cartilage matrix is composed of 2 types of macromolecules. They are the following: glycoproteids which make cartilage resistant to pressure and collagen which makes cartilage resistant to stretching and shifting. Normally, the process of formation of a new cartilage includes a number of processes involving breakdown of some substances.
1. Interleukin-1 stimulates breakdown of cartilage. Low concentrations of interleukin-1 contribute to slowing-down of regenerative processes in the cartilage matrix and inhibition of synthesis of glykoproteids in chondrocytes. Chondrocyte metabolism is affected not only by cytokines and other mediators but also by constant mechanical load on the cartilage. Static and prolonged mechanical load contribute to inhibition of synthesis of glykoproteids and proteins. On the contrary, short-term mechanical load can stimulate biosynthesis of the cartilage matrix.
2. Loss of glycosaminoglycans, such as chondroitin sulfate, keratan sulfate and hyaluronic acid in the superficial, intermediate and deep areas of the cartilage matrix is considered to be a common feature of cartilage destruction in osteoarthrosis.
The initial disease process begins with changes of the articular cartilage. One of the earliest changes of the cartilage matrix is improper direction and size of collagen fibers and their impaired connection resulting in destruction of the collagen network.
3. Lysosomal enzymes, plasmin and metalloproteinases play a major role in destruction of the cartilage matrix. And it doesn’t matter which factors stimulated their synthesis and release.
4. The main reason for the development of osteoarthrosis is disproportionate mechanical load on the articular surface of the cartilage and its ability to stand this load. As a result, degeneration and destruction of cartilage occurs.
5. Inflammation plays a significant role in pathogenesis of osteoarthrosis. The causes of inflammation have not been studied yet. Production of inflammatory cytokines, such as interleukin (IL-1, IL-6), tumor necrosis factor-alpha, etc., induces inflammation resulting in degeneration of cartilage. Inflammatory cytokines contribute to release of enzymes that destroy proteoglycan and collagen (e.g. collagenase, stromelysin). They also contribute to an increased production of prostaglandins and activators of plasminogen
This plays a significant role in inflammation and pain sensation modeling. Some products of inflammation, such as bradykinin and histamine, can stimulate primary afferent nerve fibers, while others, such as prostaglandins, leukotrienes and interleukins IL-1-beta, IL-6, can increase susceptibility of these fibers to various exogenous irritants.
Once biologically active substances have been released, they cause inflammation in tissues of the joint with a subsequent destruction of the synovial membrane of the joint resulting in progressing synovitis and increased production of inflammatory cytokines. Proteoglycans which are considered to be the products of breakdown of chondrocytes and collagen are referred to as antigens which can induce production of autoantibodies with a subsequent development of local inflammation.
6. A well-marked induced form of synthetase of nitric oxide [NO] can contribute to an increased production of nitric oxide which has a toxic effect on cartilage.
7. Immunological aspects of pathogenesis.
1) Some parts of cartilage have antigenic features and may serve as a source of autoimmune reactions.
2) Detection of immune complexes in the affected cartilage as well as circulating antibodies to proteoglycans of the cartilage at an early stage of osteoarthrosis indicates great significance of immune reactions for these components in pathogenesis of osteoarthrosis.
3) The extent of destruction of cartilage has an effect on immune responses to proteoglycans.
4) Antibodies to glucosaminoglycanes participate in destruction of cartilage in osteoarthrosis.
8. Reduction processes.
Cartilage involvement triggers proliferation of chondrocytes and increased synthesis of proteoglycans. Tissue inhibitors of metalloproteinases and antiactivators of plasminogen 1 can stabilize the cartilage. Transforming growth factor-beta and fibroblast growth factor contribute to regeneration of cartilage.
1) In osteoarthrosis chondrocytes proliferate actively and produce great amounts of nucleic acid, glycoproteids, collagen and other proteins. Therefore, the term degenerative joint disease is no longer appropriate when referring to OA.
2) High activity of chondrocytes can lead to an increased concentration of glycoproteids and thickening of cartilage. However, regenerative tissue is less resistant to mechanical load than true cartilage.
5. Mechanical factors.
1) Loss of proteoglycanes leads to decreased elasticity of cartilage and transfer of mechanical load onto chondrocytes.
2) In subchondral osteosclerosis mechanical load is also transferred onto chondrocytes.
Pathomorphology.
The following changes occur in cartilage in osteoarthrosis:
1) At an early stage of osteoarthrosis the colour of cartilage changes resulting from loss of proteoglycans.
2) The cartilage matrix of the superficial layer becomes poor in proteoglycans resulting in its dehydration. At the same time we can observe necrosis of some chondrocytes as well as disorganization and sclerosis of collagen fibrils.
3) Local areas of cartilage softening are early signs of osteoarthrosis. Later in life fibrillation and erosion of the articular surface occurs. Collagen fragments, fibrillation and erosion of the articular surface are typical of the disease.
4) In deeper layers of cartilage in addition to necrosis of chondrocytes some reactive changes, such as hyperplasia and proliferation of chondrocytes with a subsequent increase of synthesis of proteoglycans, occur. These changes precede cartilage destruction and occur in the area that bear weight.
5) Vertical cracks of cartilage reaching the subchondral bone are observed at an extentsive stage of the disease. They indicate that the disease progresses quickly. Ulcers are typically observed and the bone becomes exposed.
6) Erosion causes cartilage thinning.
Changes occurring in bone:
1) Bone tissue neoplasms. The presence of osteosclerosis in subchondral bone and osteophytes (or spurs) at the joint margins are the most characteristic X-ray findings. The bone under the ulcerated cartilage is similar to ivory. This process is called eburnation. Osteophytes cause the joint to change its shape and along with chronic focal synovitis and articular capsule thickening can limit the range of motion of the joint. As a result, atrophy of paraarticular muscles occurs. It can play a significant role in detecting clinical manifestations and determining the extent of lack of productivity.
2) Subchondral cysts.
They usually occur on the articular surface of bones resulting from transfer of mechanical load from cartilage onto bone. Insufficient blood supply makes difficult their resorption.
Types of osteoarthrosis
I. According to aetiologic factors, the following types of osteoarthrosis are singled out:
A) Primary osteoarthrosis involves any healthy joints.
It is subdivided into the following subtypes:
1) Primary osteoarthrosis, which affects one or several joints. The most commonly affected joints are the following:
(a) Carpometacarpal joint involvement: Herberden
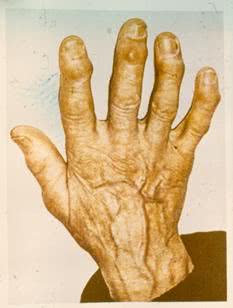 or Bouchard nodes (nodular osteoarthritis deformans),
or Bouchard nodes (nodular osteoarthritis deformans),
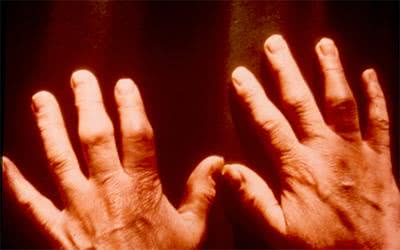 erosive osteoarthrosis of interphalangeal joints (without nodules), osteoarthrosis of the first carpometacarpal joint.
(b) Foot involvement: valgus deformation of the big toe, stiffness of the 1st degree of metatarsophalangeal joint, hammer toes, osteoarthrosis of talocalcaneonavicular joint.
erosive osteoarthrosis of interphalangeal joints (without nodules), osteoarthrosis of the first carpometacarpal joint.
(b) Foot involvement: valgus deformation of the big toe, stiffness of the 1st degree of metatarsophalangeal joint, hammer toes, osteoarthrosis of talocalcaneonavicular joint.
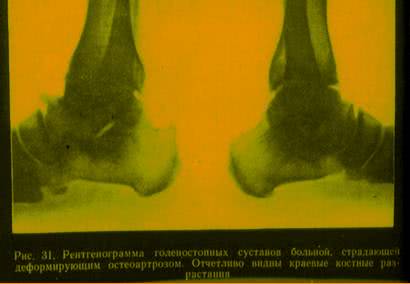 (c) Knee involvement: deforming ostoeoarthrosis, osteoarthrosis of external femorotibial joint; osteoarthrosis of femoropatellar joint.
(d) Hip involvement: marginal osteoarthrosis (changes of the upper margin of cotyloid cavity); central (axial, medial) osteoarthrosis; diffusive deforming osteoarthrosis (coxae senilis).
(e) Spine involvement: involvement of intervertebral joints (deforming osteoarthrosis); involvement of intervertebral disks (osteochondrosis); osteophytes (osteochondrosis); ligament involvement (diffusive hyperostosis).
f) Impairment of other joints: shoulder, acromioclavicular joint, ankle, sacroiliac joint, temporomandibular joint.
2) General deforming ostearthrosis. It affects 3 or more joints which are mentioned above.
B) Secondary osteoarthrosis may affect joints that are generally involved with primary osteoarthrosis.
1) Trauma: acute or chronic (for example, occupational trauma, sports-related injury, etc.).
2) Congenital diseases:
(a) Local lesions: osteochondropathy of the femoral head, congenital dislocation of the femoral bone.
(b) Biomechanical disorders: different length of legs, knock knee (genu valgum) and bowleg knee (genu varum), hypermobility of joints.
(c) Chondrodisplasia: epiphisal chondrodisplasia, spondiloepiphisal chondrodisplasia, etc.
3) Metabolic disturbances: hemochromatosis, Wilson’s disease, alkaptonuria, Gaucher’s disease.
4) Endocrine diseases: (acromegaly, diabetes mellitus, hyperparathyroidism, hypothyroidism and obesity).
5) Calcium pyrophosphate deposits: pseudopodagra, apatite disease.
6) Other diseases of bones and joints:
(a) Local: fracture, gout, infection, and aseptic necrosis.
(b) General: Padgett’s disease, osteoporosis, osteochondritis, rheumatoid arthritis.
7) Neurogenic arthropathy.
8 Endemic diseases: Kashin – Bek disease, Mseliny disease.
9) Other factors: frostbite, decompression disease, haemoglobinopathy.
II. According to the extent of disease progression, the following types of osteoarthrosis are singled out:
a) Without well-marked progression.
b) Slow disease progression.
c) Well marked disease progression.
III. According to the presence of synovitis, the following types of osteoarthrosis are singled out:
a) OA, which is not associated with reactive synovitis;
b) OA associated with reactive synovitis;
c) OA associated with recurrent synovitis.
IV. According to the extent of disorder of joint function, the following stages are singled out:
0 stage – 1st stage – 2nd stage – 3 stage
Clinical manifestations: Clinical manifestations depend on the number of affected joints and the severity of the disease.
Osteoarthrosis usually develops slowly over time and may result in several problems, such as short-term and slight pain in weight bearing joints.
(c) Knee involvement: deforming ostoeoarthrosis, osteoarthrosis of external femorotibial joint; osteoarthrosis of femoropatellar joint.
(d) Hip involvement: marginal osteoarthrosis (changes of the upper margin of cotyloid cavity); central (axial, medial) osteoarthrosis; diffusive deforming osteoarthrosis (coxae senilis).
(e) Spine involvement: involvement of intervertebral joints (deforming osteoarthrosis); involvement of intervertebral disks (osteochondrosis); osteophytes (osteochondrosis); ligament involvement (diffusive hyperostosis).
f) Impairment of other joints: shoulder, acromioclavicular joint, ankle, sacroiliac joint, temporomandibular joint.
2) General deforming ostearthrosis. It affects 3 or more joints which are mentioned above.
B) Secondary osteoarthrosis may affect joints that are generally involved with primary osteoarthrosis.
1) Trauma: acute or chronic (for example, occupational trauma, sports-related injury, etc.).
2) Congenital diseases:
(a) Local lesions: osteochondropathy of the femoral head, congenital dislocation of the femoral bone.
(b) Biomechanical disorders: different length of legs, knock knee (genu valgum) and bowleg knee (genu varum), hypermobility of joints.
(c) Chondrodisplasia: epiphisal chondrodisplasia, spondiloepiphisal chondrodisplasia, etc.
3) Metabolic disturbances: hemochromatosis, Wilson’s disease, alkaptonuria, Gaucher’s disease.
4) Endocrine diseases: (acromegaly, diabetes mellitus, hyperparathyroidism, hypothyroidism and obesity).
5) Calcium pyrophosphate deposits: pseudopodagra, apatite disease.
6) Other diseases of bones and joints:
(a) Local: fracture, gout, infection, and aseptic necrosis.
(b) General: Padgett’s disease, osteoporosis, osteochondritis, rheumatoid arthritis.
7) Neurogenic arthropathy.
8 Endemic diseases: Kashin – Bek disease, Mseliny disease.
9) Other factors: frostbite, decompression disease, haemoglobinopathy.
II. According to the extent of disease progression, the following types of osteoarthrosis are singled out:
a) Without well-marked progression.
b) Slow disease progression.
c) Well marked disease progression.
III. According to the presence of synovitis, the following types of osteoarthrosis are singled out:
a) OA, which is not associated with reactive synovitis;
b) OA associated with reactive synovitis;
c) OA associated with recurrent synovitis.
IV. According to the extent of disorder of joint function, the following stages are singled out:
0 stage – 1st stage – 2nd stage – 3 stage
Clinical manifestations: Clinical manifestations depend on the number of affected joints and the severity of the disease.
Osteoarthrosis usually develops slowly over time and may result in several problems, such as short-term and slight pain in weight bearing joints.

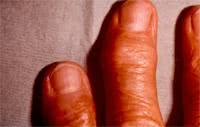 Distal and proximal interphalangeal joints and the first carpometacarpal joint are most commonly affected.
Distal and proximal interphalangeal joints and the first carpometacarpal joint are most commonly affected.
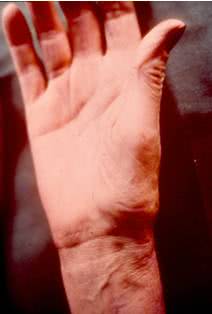 The mechanism of pain in osteoarthrosis is complicated and has not been studied yet.
Most patients suffer from deep and dull pain, which gets worse on physical exertion and is relieved at rest. As the disease progresses, the pain becomes more intensive and prolonged. The patient may have pain when moving a joint and even at rest. The pain usually gets worse at night and may interfere with sleep.
Possible causes of pain:
The mechanism of pain in osteoarthrosis is complicated and has not been studied yet.
Most patients suffer from deep and dull pain, which gets worse on physical exertion and is relieved at rest. As the disease progresses, the pain becomes more intensive and prolonged. The patient may have pain when moving a joint and even at rest. The pain usually gets worse at night and may interfere with sleep.
Possible causes of pain:
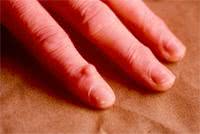 A local increase of body temperature is not typical of osteoarthrosis, however the person may have high temperature in aggravation of the disease. Fibrosis of the synovium and the articular capsule contributes to sprain of ligaments and muscular hypotonia resulting in subluxations.
Limitation of joint motion can occur in disease progression due to pain syndrome, reflex muscle spasm, formation of tendomuscular contractures and osteophytes, entrapment of the sequestrum of cartilage, presence of subluxations. Restriction of joint movement may occur in one direction of the affected joint. The range of motions in other directions may not be reduced.
Imaging Studies.
The following characteristic findings are typically observed at the 1st stage of osteoarthrosis:
1) Sclerosis and dilatation of terminal bone lamella.
2) Other findings at this stage include joint space narrowing which is typically not so great (less than 50%). However, X-ray findings at an early stage are often poor predictors of the degree of cartilage involvement, as they consider only the width of joint space.
3) Absence of osteophytes (spurs at the joint margins) and articular surfaces can be seen very well.
The following characteristic findings are typically observed at the 2nd stage of osteoarthrosis:
1) Joint space narrowing is typically more than 50 %.
2) Cyst formation on subchondral bone.
3) Subchondral bone sclerosis.
4) Presence of osteophytes in the form of thorns.
The following characteristic findings are typically observed at the 3rd stage of osteoarthrosis:
1) Great asymmetric joint space narrowing.
2) Deformation of epiphysis.
3) Large spurs at the joint margins.
4) Asymmetric articular surfaces.
5) Occasionally, hypertrophy of the villi of the synovial membrane whose avulsion may result in entrapment of the sequestrum of cartilage.
The following characteristic findings are typically observed at the 4th stage of osteoarthrosis:
1) Well marked joint space narrowing due to loss of cartilage.
2) Presence of a great number of osteophytes.
Lab Studies: No specific laboratory abnormalities are associated with osteoarthrosis, however, laboratory studies can help detect the cause of secondary osteoarthrosis. In primary osteoarthrosis total and biochemical blood and urine analyses are not elevated. Synovial fluid analysis usually indicates a white cell count less than 2000 per mm3.
It is usually turbid and viscous. Synovial fluid analysis helps differentiate osteoarthrosis from pseudogout, gout and infectious arthritis. In synovitis some hematologic findings can occur.
Main Clinical Forms.
40% of cases show coxarthrosis which is one of the main types of osteoarthrosis. Patients may have rapid fatigability of hip muscles, pain after joint use in the inguinal region, hip, buttock and ocassionally in the knee.
A local increase of body temperature is not typical of osteoarthrosis, however the person may have high temperature in aggravation of the disease. Fibrosis of the synovium and the articular capsule contributes to sprain of ligaments and muscular hypotonia resulting in subluxations.
Limitation of joint motion can occur in disease progression due to pain syndrome, reflex muscle spasm, formation of tendomuscular contractures and osteophytes, entrapment of the sequestrum of cartilage, presence of subluxations. Restriction of joint movement may occur in one direction of the affected joint. The range of motions in other directions may not be reduced.
Imaging Studies.
The following characteristic findings are typically observed at the 1st stage of osteoarthrosis:
1) Sclerosis and dilatation of terminal bone lamella.
2) Other findings at this stage include joint space narrowing which is typically not so great (less than 50%). However, X-ray findings at an early stage are often poor predictors of the degree of cartilage involvement, as they consider only the width of joint space.
3) Absence of osteophytes (spurs at the joint margins) and articular surfaces can be seen very well.
The following characteristic findings are typically observed at the 2nd stage of osteoarthrosis:
1) Joint space narrowing is typically more than 50 %.
2) Cyst formation on subchondral bone.
3) Subchondral bone sclerosis.
4) Presence of osteophytes in the form of thorns.
The following characteristic findings are typically observed at the 3rd stage of osteoarthrosis:
1) Great asymmetric joint space narrowing.
2) Deformation of epiphysis.
3) Large spurs at the joint margins.
4) Asymmetric articular surfaces.
5) Occasionally, hypertrophy of the villi of the synovial membrane whose avulsion may result in entrapment of the sequestrum of cartilage.
The following characteristic findings are typically observed at the 4th stage of osteoarthrosis:
1) Well marked joint space narrowing due to loss of cartilage.
2) Presence of a great number of osteophytes.
Lab Studies: No specific laboratory abnormalities are associated with osteoarthrosis, however, laboratory studies can help detect the cause of secondary osteoarthrosis. In primary osteoarthrosis total and biochemical blood and urine analyses are not elevated. Synovial fluid analysis usually indicates a white cell count less than 2000 per mm3.
It is usually turbid and viscous. Synovial fluid analysis helps differentiate osteoarthrosis from pseudogout, gout and infectious arthritis. In synovitis some hematologic findings can occur.
Main Clinical Forms.
40% of cases show coxarthrosis which is one of the main types of osteoarthrosis. Patients may have rapid fatigability of hip muscles, pain after joint use in the inguinal region, hip, buttock and ocassionally in the knee.
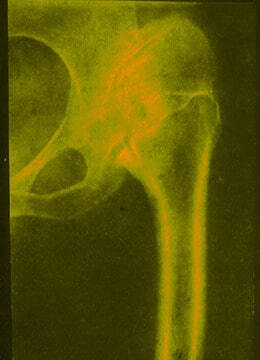 Pain can become persistent and it gets worse, especially when moving a joint. Sometimes the hip joint gets locked. Patients may develop atrophy of muscles of the hip and buttocks.
Pain is often associated with limping, which is mainly caused by muscle spasm and deformity of the femoral head, its protrusion into the fossa of the iliac bone (in case of subluxation). It often results in shortening of the leg. When the hip is involved, patients typically have waddling (or goose) gait.
Gonarthrosis is the most common type of osteoarthrosis. It is typically bilateral. In gonarthrosis internal and external femorotibial and femoropatellar joints are involved.
Pain can become persistent and it gets worse, especially when moving a joint. Sometimes the hip joint gets locked. Patients may develop atrophy of muscles of the hip and buttocks.
Pain is often associated with limping, which is mainly caused by muscle spasm and deformity of the femoral head, its protrusion into the fossa of the iliac bone (in case of subluxation). It often results in shortening of the leg. When the hip is involved, patients typically have waddling (or goose) gait.
Gonarthrosis is the most common type of osteoarthrosis. It is typically bilateral. In gonarthrosis internal and external femorotibial and femoropatellar joints are involved.
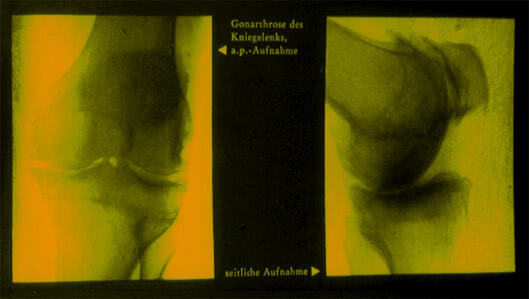 Mechanical pain localized at the anterior and internal surfaces of the joint is the most important clinical characteristic of gonarthrosis. The pain in the knee develops gradually over time and it gets worse, especially when walking, standing or going downhill. It irradiates to the hip and shin and can be relieved by rest at night. These changes can cause restriction of joint movement, its extension and flexion.
Herberden form of osteoarthrosis is referred to as arthrosis of distal interphalangial joints. It is more common in women. The onset of the disease may be asymptomatic. Initially, symptomatic patients develop joint stiffness resulting in swelling of soft tissues of the joint in dorsal and lateral areas on one side or both sides of the joint. It can be painful when palpated. These changes happen slowly over time and the swelling turns into Herberden nodes. Herberden nodes are dense, multiple, symmetric substances which cause the joint to distort.
Reactive synovitis can occur in patients who have painful and swollen nodes. These changes cannot be observed in any other types of arthrosis.
Arthrosis associated with Bouchard nodes is referred to as arthrosis of proximal interphalangial joints. 50% of adults with Herberden nodes have Bouchard nodes. It usually affects several joints. Patients with Bouchard nodes do not have pain. Osteoarthrosis of interphalangial joints can lead to well marked deformity of joints and their increased size. Bourchard nodes are usually localized at the lateral surface of a joint. The finger usually takes a fusiform shape due to deformity of a joint. The range of motion of the affected joint is limited.
Osteoarthrosis of the first carpometacarpal joint ranks the second among the most common types of osteoarthrosis. In comparison with Herberden nodes, this type of osteoarthrosis is characterised by swollen and painful joints, crepitus, joint stiffness and muscle weakness. Osteophytes cause the joint to take an anglar shape. The patient often feels pain which makes the patient to press the thumb to the palm. Compensatory overextension of the first metacarpophalangial joint usually occurs; the finger is distorted and looks like a “swan neck”.
Osteoarthrosis of the elbow occurs less commonly than other types of osteoarthrosis. It is characterised by osteophyte formation at the joint margins and around the articular surface of the ulnar bone leading to restriction of joint movement.
Osteoarthrosis of the shoulder is characterized by subacromial joint involvement resulting in painful abduction of the shoulder and reduced range of motion. Arthrosis of the shoulder proper occurs less commonly. In this case the shoulder joint is not distorted.
Mechanical pain localized at the anterior and internal surfaces of the joint is the most important clinical characteristic of gonarthrosis. The pain in the knee develops gradually over time and it gets worse, especially when walking, standing or going downhill. It irradiates to the hip and shin and can be relieved by rest at night. These changes can cause restriction of joint movement, its extension and flexion.
Herberden form of osteoarthrosis is referred to as arthrosis of distal interphalangial joints. It is more common in women. The onset of the disease may be asymptomatic. Initially, symptomatic patients develop joint stiffness resulting in swelling of soft tissues of the joint in dorsal and lateral areas on one side or both sides of the joint. It can be painful when palpated. These changes happen slowly over time and the swelling turns into Herberden nodes. Herberden nodes are dense, multiple, symmetric substances which cause the joint to distort.
Reactive synovitis can occur in patients who have painful and swollen nodes. These changes cannot be observed in any other types of arthrosis.
Arthrosis associated with Bouchard nodes is referred to as arthrosis of proximal interphalangial joints. 50% of adults with Herberden nodes have Bouchard nodes. It usually affects several joints. Patients with Bouchard nodes do not have pain. Osteoarthrosis of interphalangial joints can lead to well marked deformity of joints and their increased size. Bourchard nodes are usually localized at the lateral surface of a joint. The finger usually takes a fusiform shape due to deformity of a joint. The range of motion of the affected joint is limited.
Osteoarthrosis of the first carpometacarpal joint ranks the second among the most common types of osteoarthrosis. In comparison with Herberden nodes, this type of osteoarthrosis is characterised by swollen and painful joints, crepitus, joint stiffness and muscle weakness. Osteophytes cause the joint to take an anglar shape. The patient often feels pain which makes the patient to press the thumb to the palm. Compensatory overextension of the first metacarpophalangial joint usually occurs; the finger is distorted and looks like a “swan neck”.
Osteoarthrosis of the elbow occurs less commonly than other types of osteoarthrosis. It is characterised by osteophyte formation at the joint margins and around the articular surface of the ulnar bone leading to restriction of joint movement.
Osteoarthrosis of the shoulder is characterized by subacromial joint involvement resulting in painful abduction of the shoulder and reduced range of motion. Arthrosis of the shoulder proper occurs less commonly. In this case the shoulder joint is not distorted.
 Some patients may develop moderate atrophy of the surrounding muscles. Abduction of muscles is usually impaired.
Osteoarthrosis of the sternoclavicular joint is a common lesion and is often associated with humeroscapular periarthritis. It is clinically characterised by swelling, deformity of a joint and pain on movement. Osteoarthrosis of the sternoclavicular joint may be related to arthritis.
Osteoarthrosis of the ankle is never primary. It is often secondary to injury. It causes reduced range of motion of a joint and restriction of motor activity resulting in lack of productivity.
Osteoarthrosis of the 1st metatarsophalangial joint occurs most frequently and is typically associated with impaired static position, such as transverse or longitudinal platypodia, injury or occupational overload. It is characterised by tenderness, restriction of movement of the big toe, difficulty in walking. Transverse platypodia causes the big toe to incline outside resulting in hallux valgus and chronic bursitis of the first toe. Subluxation and dislocation of the head of metatarsal bone occurs quite often.
Polyosteoarthrosis is characterised by multiple lesions of peripheral and intervertebral joints.
It is clinically characterised by arthrosis, diskopathy and numerous tendopathies. Joint lesions are typically bilateral and symmetric. Weight-bearing joints, such as hip, knee and distal interphalangeal joints, are commonly affected. Joints of the big toe, thumb and ankle are less commonly affected.
Degenerate-dystrophic changes of spine joints are also referred to as osteoarthrosis.
Some patients may develop moderate atrophy of the surrounding muscles. Abduction of muscles is usually impaired.
Osteoarthrosis of the sternoclavicular joint is a common lesion and is often associated with humeroscapular periarthritis. It is clinically characterised by swelling, deformity of a joint and pain on movement. Osteoarthrosis of the sternoclavicular joint may be related to arthritis.
Osteoarthrosis of the ankle is never primary. It is often secondary to injury. It causes reduced range of motion of a joint and restriction of motor activity resulting in lack of productivity.
Osteoarthrosis of the 1st metatarsophalangial joint occurs most frequently and is typically associated with impaired static position, such as transverse or longitudinal platypodia, injury or occupational overload. It is characterised by tenderness, restriction of movement of the big toe, difficulty in walking. Transverse platypodia causes the big toe to incline outside resulting in hallux valgus and chronic bursitis of the first toe. Subluxation and dislocation of the head of metatarsal bone occurs quite often.
Polyosteoarthrosis is characterised by multiple lesions of peripheral and intervertebral joints.
It is clinically characterised by arthrosis, diskopathy and numerous tendopathies. Joint lesions are typically bilateral and symmetric. Weight-bearing joints, such as hip, knee and distal interphalangeal joints, are commonly affected. Joints of the big toe, thumb and ankle are less commonly affected.
Degenerate-dystrophic changes of spine joints are also referred to as osteoarthrosis.
 These changes usually occur in the lumbar and cervical parts of the spine. Depending on localization, changes are manifested clinically by spastic, neurologic and vegetative disorders. Patients usually have pain and joint stiffness in different parts of the spine as well as pain syndrome which is similar to secondary radiculitis. Spasm of paravertebral muscles occurs quite often. Compression of nerve roots causes either radicular pain or paresthesia, weakening of reflexes and disorders of motor activity. Compression of the vertebral artery may cause cerebral blood flow disturbances which are clinically manifested by dizziness, headache and vision disorders (blurring, diplopia, narrowing of visual fields and scotoms).
The above mentioned neural disorders are usually periodical and paroxysmal. Neural disorders may be caused by movements of the neck or by a certain position of the neck (for example, when vertebral arteries are compressed by osteophytes). Typical features of neural disorders are pain syndrome due to compression of nerve roots and acute, sharp pain which is similar to current going through the body. The pain usually spreads downwards, aggravating during activity. It is often associated with hyperethesia or paresthesia in distal parts of the human body. In proximal parts of the body patients often have pain. Sense and movement disorders as well as changes of reflexes are observed less commonly. Movement disorders associated with weakness, hypertrophy and hypotonia may also occur. Hyporeflexia is most commonly observed on one side of the body.
Diagnosis. Osteoarthrosis can be easily diagnosed at the extensive stage.
These changes usually occur in the lumbar and cervical parts of the spine. Depending on localization, changes are manifested clinically by spastic, neurologic and vegetative disorders. Patients usually have pain and joint stiffness in different parts of the spine as well as pain syndrome which is similar to secondary radiculitis. Spasm of paravertebral muscles occurs quite often. Compression of nerve roots causes either radicular pain or paresthesia, weakening of reflexes and disorders of motor activity. Compression of the vertebral artery may cause cerebral blood flow disturbances which are clinically manifested by dizziness, headache and vision disorders (blurring, diplopia, narrowing of visual fields and scotoms).
The above mentioned neural disorders are usually periodical and paroxysmal. Neural disorders may be caused by movements of the neck or by a certain position of the neck (for example, when vertebral arteries are compressed by osteophytes). Typical features of neural disorders are pain syndrome due to compression of nerve roots and acute, sharp pain which is similar to current going through the body. The pain usually spreads downwards, aggravating during activity. It is often associated with hyperethesia or paresthesia in distal parts of the human body. In proximal parts of the body patients often have pain. Sense and movement disorders as well as changes of reflexes are observed less commonly. Movement disorders associated with weakness, hypertrophy and hypotonia may also occur. Hyporeflexia is most commonly observed on one side of the body.
Diagnosis. Osteoarthrosis can be easily diagnosed at the extensive stage.
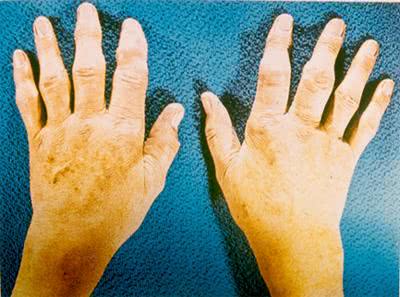 Clinical history and characteristic radiographic findings can help differentiate osteoarthrosis from other conditions.
Diagnostic criteria of osteoarthrosis:
Clinical history and characteristic radiographic findings can help differentiate osteoarthrosis from other conditions.
Diagnostic criteria of osteoarthrosis:
The first two clinical and radiographic criteria must be present to make a diagnosis of osteoarthrosis.
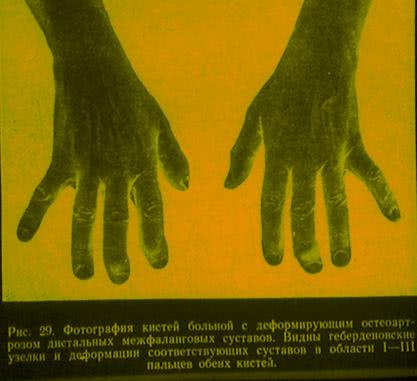
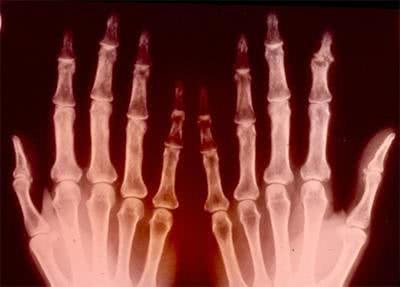 Differentiation of Osteoarthritis from Other Diseases.
Imaging studies of the affected joint are usually conducted in the elderly who may not have any other clinical features. For making a final diagnosis we cannot rely only on imaging or laboratory findings.
A comprehensive analysis of clinical manifestations and some additional studies may be necessary for detecting the causes of pain in joints.
Osteoarthrosis must be differentiated from arthritis of various origin, such as:
1.Rheumatoid arthritis. It should be remembered that osteoarthrosis is often associated with rheumatoid arthritis.
2. Gout.
3. Ankylosing spondylitis.
4. Diffuse hyperstosis.
5. Rheumatic polyarthritis.
Treatment of Osteoarthrosis.
Treatment of osteoarthrosis must be complex and should be undertaken considering various aetiological and pathogenetic factors which can vary. Effectiveness of treatment depends on the stage of the disease. Presence or absence of reactive synovitis plays a major role in selection of treatment. The course of the disease and underlying diseases may be also relevant. The main principle of treatment of osteoarthrosis which is often not observed is its duration and systematicity.
Differentiation of Osteoarthritis from Other Diseases.
Imaging studies of the affected joint are usually conducted in the elderly who may not have any other clinical features. For making a final diagnosis we cannot rely only on imaging or laboratory findings.
A comprehensive analysis of clinical manifestations and some additional studies may be necessary for detecting the causes of pain in joints.
Osteoarthrosis must be differentiated from arthritis of various origin, such as:
1.Rheumatoid arthritis. It should be remembered that osteoarthrosis is often associated with rheumatoid arthritis.
2. Gout.
3. Ankylosing spondylitis.
4. Diffuse hyperstosis.
5. Rheumatic polyarthritis.
Treatment of Osteoarthrosis.
Treatment of osteoarthrosis must be complex and should be undertaken considering various aetiological and pathogenetic factors which can vary. Effectiveness of treatment depends on the stage of the disease. Presence or absence of reactive synovitis plays a major role in selection of treatment. The course of the disease and underlying diseases may be also relevant. The main principle of treatment of osteoarthrosis which is often not observed is its duration and systematicity.




 or Bouchard nodes (nodular osteoarthritis deformans),
or Bouchard nodes (nodular osteoarthritis deformans),
 erosive osteoarthrosis of interphalangeal joints (without nodules), osteoarthrosis of the first carpometacarpal joint.
(b) Foot involvement: valgus deformation of the big toe, stiffness of the 1st degree of metatarsophalangeal joint, hammer toes, osteoarthrosis of talocalcaneonavicular joint.
erosive osteoarthrosis of interphalangeal joints (without nodules), osteoarthrosis of the first carpometacarpal joint.
(b) Foot involvement: valgus deformation of the big toe, stiffness of the 1st degree of metatarsophalangeal joint, hammer toes, osteoarthrosis of talocalcaneonavicular joint.
 (c) Knee involvement: deforming ostoeoarthrosis, osteoarthrosis of external femorotibial joint; osteoarthrosis of femoropatellar joint.
(d) Hip involvement: marginal osteoarthrosis (changes of the upper margin of cotyloid cavity); central (axial, medial) osteoarthrosis; diffusive deforming osteoarthrosis (coxae senilis).
(e) Spine involvement: involvement of intervertebral joints (deforming osteoarthrosis); involvement of intervertebral disks (osteochondrosis); osteophytes (osteochondrosis); ligament involvement (diffusive hyperostosis).
f) Impairment of other joints: shoulder, acromioclavicular joint, ankle, sacroiliac joint, temporomandibular joint.
2) General deforming ostearthrosis. It affects 3 or more joints which are mentioned above.
B) Secondary osteoarthrosis may affect joints that are generally involved with primary osteoarthrosis.
1) Trauma: acute or chronic (for example, occupational trauma, sports-related injury, etc.).
2) Congenital diseases:
(a) Local lesions: osteochondropathy of the femoral head, congenital dislocation of the femoral bone.
(b) Biomechanical disorders: different length of legs, knock knee (genu valgum) and bowleg knee (genu varum), hypermobility of joints.
(c) Chondrodisplasia: epiphisal chondrodisplasia, spondiloepiphisal chondrodisplasia, etc.
3) Metabolic disturbances: hemochromatosis, Wilson’s disease, alkaptonuria, Gaucher’s disease.
4) Endocrine diseases: (acromegaly, diabetes mellitus, hyperparathyroidism, hypothyroidism and obesity).
5) Calcium pyrophosphate deposits: pseudopodagra, apatite disease.
6) Other diseases of bones and joints:
(a) Local: fracture, gout, infection, and aseptic necrosis.
(b) General: Padgett’s disease, osteoporosis, osteochondritis, rheumatoid arthritis.
7) Neurogenic arthropathy.
8 Endemic diseases: Kashin – Bek disease, Mseliny disease.
9) Other factors: frostbite, decompression disease, haemoglobinopathy.
II. According to the extent of disease progression, the following types of osteoarthrosis are singled out:
a) Without well-marked progression.
b) Slow disease progression.
c) Well marked disease progression.
III. According to the presence of synovitis, the following types of osteoarthrosis are singled out:
a) OA, which is not associated with reactive synovitis;
b) OA associated with reactive synovitis;
c) OA associated with recurrent synovitis.
IV. According to the extent of disorder of joint function, the following stages are singled out:
0 stage – 1st stage – 2nd stage – 3 stage
Clinical manifestations: Clinical manifestations depend on the number of affected joints and the severity of the disease.
Osteoarthrosis usually develops slowly over time and may result in several problems, such as short-term and slight pain in weight bearing joints.
(c) Knee involvement: deforming ostoeoarthrosis, osteoarthrosis of external femorotibial joint; osteoarthrosis of femoropatellar joint.
(d) Hip involvement: marginal osteoarthrosis (changes of the upper margin of cotyloid cavity); central (axial, medial) osteoarthrosis; diffusive deforming osteoarthrosis (coxae senilis).
(e) Spine involvement: involvement of intervertebral joints (deforming osteoarthrosis); involvement of intervertebral disks (osteochondrosis); osteophytes (osteochondrosis); ligament involvement (diffusive hyperostosis).
f) Impairment of other joints: shoulder, acromioclavicular joint, ankle, sacroiliac joint, temporomandibular joint.
2) General deforming ostearthrosis. It affects 3 or more joints which are mentioned above.
B) Secondary osteoarthrosis may affect joints that are generally involved with primary osteoarthrosis.
1) Trauma: acute or chronic (for example, occupational trauma, sports-related injury, etc.).
2) Congenital diseases:
(a) Local lesions: osteochondropathy of the femoral head, congenital dislocation of the femoral bone.
(b) Biomechanical disorders: different length of legs, knock knee (genu valgum) and bowleg knee (genu varum), hypermobility of joints.
(c) Chondrodisplasia: epiphisal chondrodisplasia, spondiloepiphisal chondrodisplasia, etc.
3) Metabolic disturbances: hemochromatosis, Wilson’s disease, alkaptonuria, Gaucher’s disease.
4) Endocrine diseases: (acromegaly, diabetes mellitus, hyperparathyroidism, hypothyroidism and obesity).
5) Calcium pyrophosphate deposits: pseudopodagra, apatite disease.
6) Other diseases of bones and joints:
(a) Local: fracture, gout, infection, and aseptic necrosis.
(b) General: Padgett’s disease, osteoporosis, osteochondritis, rheumatoid arthritis.
7) Neurogenic arthropathy.
8 Endemic diseases: Kashin – Bek disease, Mseliny disease.
9) Other factors: frostbite, decompression disease, haemoglobinopathy.
II. According to the extent of disease progression, the following types of osteoarthrosis are singled out:
a) Without well-marked progression.
b) Slow disease progression.
c) Well marked disease progression.
III. According to the presence of synovitis, the following types of osteoarthrosis are singled out:
a) OA, which is not associated with reactive synovitis;
b) OA associated with reactive synovitis;
c) OA associated with recurrent synovitis.
IV. According to the extent of disorder of joint function, the following stages are singled out:
0 stage – 1st stage – 2nd stage – 3 stage
Clinical manifestations: Clinical manifestations depend on the number of affected joints and the severity of the disease.
Osteoarthrosis usually develops slowly over time and may result in several problems, such as short-term and slight pain in weight bearing joints.

 Distal and proximal interphalangeal joints and the first carpometacarpal joint are most commonly affected.
Distal and proximal interphalangeal joints and the first carpometacarpal joint are most commonly affected.
 The mechanism of pain in osteoarthrosis is complicated and has not been studied yet.
Most patients suffer from deep and dull pain, which gets worse on physical exertion and is relieved at rest. As the disease progresses, the pain becomes more intensive and prolonged. The patient may have pain when moving a joint and even at rest. The pain usually gets worse at night and may interfere with sleep.
Possible causes of pain:
The mechanism of pain in osteoarthrosis is complicated and has not been studied yet.
Most patients suffer from deep and dull pain, which gets worse on physical exertion and is relieved at rest. As the disease progresses, the pain becomes more intensive and prolonged. The patient may have pain when moving a joint and even at rest. The pain usually gets worse at night and may interfere with sleep.
Possible causes of pain:
- Synovitis. In synovitis the synovial membrane stretches and the synovial villi are entrapped.
- Muscle spasm.
- Tendobursitis.
- Friction of the affected cartilage.
- Reflex irradiation of pain in the knee in coxitis.
- Decreased sensivity to physical /mechanical load.
- Fibrosis of the synovium and the articular capsule.
- Inflammation in and around a joint.
- Passive hyperemia of the subchondral area.
- Formation of osteophytes, which cause blockade.
 A local increase of body temperature is not typical of osteoarthrosis, however the person may have high temperature in aggravation of the disease. Fibrosis of the synovium and the articular capsule contributes to sprain of ligaments and muscular hypotonia resulting in subluxations.
Limitation of joint motion can occur in disease progression due to pain syndrome, reflex muscle spasm, formation of tendomuscular contractures and osteophytes, entrapment of the sequestrum of cartilage, presence of subluxations. Restriction of joint movement may occur in one direction of the affected joint. The range of motions in other directions may not be reduced.
Imaging Studies.
The following characteristic findings are typically observed at the 1st stage of osteoarthrosis:
1) Sclerosis and dilatation of terminal bone lamella.
2) Other findings at this stage include joint space narrowing which is typically not so great (less than 50%). However, X-ray findings at an early stage are often poor predictors of the degree of cartilage involvement, as they consider only the width of joint space.
3) Absence of osteophytes (spurs at the joint margins) and articular surfaces can be seen very well.
The following characteristic findings are typically observed at the 2nd stage of osteoarthrosis:
1) Joint space narrowing is typically more than 50 %.
2) Cyst formation on subchondral bone.
3) Subchondral bone sclerosis.
4) Presence of osteophytes in the form of thorns.
The following characteristic findings are typically observed at the 3rd stage of osteoarthrosis:
1) Great asymmetric joint space narrowing.
2) Deformation of epiphysis.
3) Large spurs at the joint margins.
4) Asymmetric articular surfaces.
5) Occasionally, hypertrophy of the villi of the synovial membrane whose avulsion may result in entrapment of the sequestrum of cartilage.
The following characteristic findings are typically observed at the 4th stage of osteoarthrosis:
1) Well marked joint space narrowing due to loss of cartilage.
2) Presence of a great number of osteophytes.
Lab Studies: No specific laboratory abnormalities are associated with osteoarthrosis, however, laboratory studies can help detect the cause of secondary osteoarthrosis. In primary osteoarthrosis total and biochemical blood and urine analyses are not elevated. Synovial fluid analysis usually indicates a white cell count less than 2000 per mm3.
It is usually turbid and viscous. Synovial fluid analysis helps differentiate osteoarthrosis from pseudogout, gout and infectious arthritis. In synovitis some hematologic findings can occur.
Main Clinical Forms.
40% of cases show coxarthrosis which is one of the main types of osteoarthrosis. Patients may have rapid fatigability of hip muscles, pain after joint use in the inguinal region, hip, buttock and ocassionally in the knee.
A local increase of body temperature is not typical of osteoarthrosis, however the person may have high temperature in aggravation of the disease. Fibrosis of the synovium and the articular capsule contributes to sprain of ligaments and muscular hypotonia resulting in subluxations.
Limitation of joint motion can occur in disease progression due to pain syndrome, reflex muscle spasm, formation of tendomuscular contractures and osteophytes, entrapment of the sequestrum of cartilage, presence of subluxations. Restriction of joint movement may occur in one direction of the affected joint. The range of motions in other directions may not be reduced.
Imaging Studies.
The following characteristic findings are typically observed at the 1st stage of osteoarthrosis:
1) Sclerosis and dilatation of terminal bone lamella.
2) Other findings at this stage include joint space narrowing which is typically not so great (less than 50%). However, X-ray findings at an early stage are often poor predictors of the degree of cartilage involvement, as they consider only the width of joint space.
3) Absence of osteophytes (spurs at the joint margins) and articular surfaces can be seen very well.
The following characteristic findings are typically observed at the 2nd stage of osteoarthrosis:
1) Joint space narrowing is typically more than 50 %.
2) Cyst formation on subchondral bone.
3) Subchondral bone sclerosis.
4) Presence of osteophytes in the form of thorns.
The following characteristic findings are typically observed at the 3rd stage of osteoarthrosis:
1) Great asymmetric joint space narrowing.
2) Deformation of epiphysis.
3) Large spurs at the joint margins.
4) Asymmetric articular surfaces.
5) Occasionally, hypertrophy of the villi of the synovial membrane whose avulsion may result in entrapment of the sequestrum of cartilage.
The following characteristic findings are typically observed at the 4th stage of osteoarthrosis:
1) Well marked joint space narrowing due to loss of cartilage.
2) Presence of a great number of osteophytes.
Lab Studies: No specific laboratory abnormalities are associated with osteoarthrosis, however, laboratory studies can help detect the cause of secondary osteoarthrosis. In primary osteoarthrosis total and biochemical blood and urine analyses are not elevated. Synovial fluid analysis usually indicates a white cell count less than 2000 per mm3.
It is usually turbid and viscous. Synovial fluid analysis helps differentiate osteoarthrosis from pseudogout, gout and infectious arthritis. In synovitis some hematologic findings can occur.
Main Clinical Forms.
40% of cases show coxarthrosis which is one of the main types of osteoarthrosis. Patients may have rapid fatigability of hip muscles, pain after joint use in the inguinal region, hip, buttock and ocassionally in the knee.
 Pain can become persistent and it gets worse, especially when moving a joint. Sometimes the hip joint gets locked. Patients may develop atrophy of muscles of the hip and buttocks.
Pain is often associated with limping, which is mainly caused by muscle spasm and deformity of the femoral head, its protrusion into the fossa of the iliac bone (in case of subluxation). It often results in shortening of the leg. When the hip is involved, patients typically have waddling (or goose) gait.
Gonarthrosis is the most common type of osteoarthrosis. It is typically bilateral. In gonarthrosis internal and external femorotibial and femoropatellar joints are involved.
Pain can become persistent and it gets worse, especially when moving a joint. Sometimes the hip joint gets locked. Patients may develop atrophy of muscles of the hip and buttocks.
Pain is often associated with limping, which is mainly caused by muscle spasm and deformity of the femoral head, its protrusion into the fossa of the iliac bone (in case of subluxation). It often results in shortening of the leg. When the hip is involved, patients typically have waddling (or goose) gait.
Gonarthrosis is the most common type of osteoarthrosis. It is typically bilateral. In gonarthrosis internal and external femorotibial and femoropatellar joints are involved.
 Mechanical pain localized at the anterior and internal surfaces of the joint is the most important clinical characteristic of gonarthrosis. The pain in the knee develops gradually over time and it gets worse, especially when walking, standing or going downhill. It irradiates to the hip and shin and can be relieved by rest at night. These changes can cause restriction of joint movement, its extension and flexion.
Herberden form of osteoarthrosis is referred to as arthrosis of distal interphalangial joints. It is more common in women. The onset of the disease may be asymptomatic. Initially, symptomatic patients develop joint stiffness resulting in swelling of soft tissues of the joint in dorsal and lateral areas on one side or both sides of the joint. It can be painful when palpated. These changes happen slowly over time and the swelling turns into Herberden nodes. Herberden nodes are dense, multiple, symmetric substances which cause the joint to distort.
Reactive synovitis can occur in patients who have painful and swollen nodes. These changes cannot be observed in any other types of arthrosis.
Arthrosis associated with Bouchard nodes is referred to as arthrosis of proximal interphalangial joints. 50% of adults with Herberden nodes have Bouchard nodes. It usually affects several joints. Patients with Bouchard nodes do not have pain. Osteoarthrosis of interphalangial joints can lead to well marked deformity of joints and their increased size. Bourchard nodes are usually localized at the lateral surface of a joint. The finger usually takes a fusiform shape due to deformity of a joint. The range of motion of the affected joint is limited.
Osteoarthrosis of the first carpometacarpal joint ranks the second among the most common types of osteoarthrosis. In comparison with Herberden nodes, this type of osteoarthrosis is characterised by swollen and painful joints, crepitus, joint stiffness and muscle weakness. Osteophytes cause the joint to take an anglar shape. The patient often feels pain which makes the patient to press the thumb to the palm. Compensatory overextension of the first metacarpophalangial joint usually occurs; the finger is distorted and looks like a “swan neck”.
Osteoarthrosis of the elbow occurs less commonly than other types of osteoarthrosis. It is characterised by osteophyte formation at the joint margins and around the articular surface of the ulnar bone leading to restriction of joint movement.
Osteoarthrosis of the shoulder is characterized by subacromial joint involvement resulting in painful abduction of the shoulder and reduced range of motion. Arthrosis of the shoulder proper occurs less commonly. In this case the shoulder joint is not distorted.
Mechanical pain localized at the anterior and internal surfaces of the joint is the most important clinical characteristic of gonarthrosis. The pain in the knee develops gradually over time and it gets worse, especially when walking, standing or going downhill. It irradiates to the hip and shin and can be relieved by rest at night. These changes can cause restriction of joint movement, its extension and flexion.
Herberden form of osteoarthrosis is referred to as arthrosis of distal interphalangial joints. It is more common in women. The onset of the disease may be asymptomatic. Initially, symptomatic patients develop joint stiffness resulting in swelling of soft tissues of the joint in dorsal and lateral areas on one side or both sides of the joint. It can be painful when palpated. These changes happen slowly over time and the swelling turns into Herberden nodes. Herberden nodes are dense, multiple, symmetric substances which cause the joint to distort.
Reactive synovitis can occur in patients who have painful and swollen nodes. These changes cannot be observed in any other types of arthrosis.
Arthrosis associated with Bouchard nodes is referred to as arthrosis of proximal interphalangial joints. 50% of adults with Herberden nodes have Bouchard nodes. It usually affects several joints. Patients with Bouchard nodes do not have pain. Osteoarthrosis of interphalangial joints can lead to well marked deformity of joints and their increased size. Bourchard nodes are usually localized at the lateral surface of a joint. The finger usually takes a fusiform shape due to deformity of a joint. The range of motion of the affected joint is limited.
Osteoarthrosis of the first carpometacarpal joint ranks the second among the most common types of osteoarthrosis. In comparison with Herberden nodes, this type of osteoarthrosis is characterised by swollen and painful joints, crepitus, joint stiffness and muscle weakness. Osteophytes cause the joint to take an anglar shape. The patient often feels pain which makes the patient to press the thumb to the palm. Compensatory overextension of the first metacarpophalangial joint usually occurs; the finger is distorted and looks like a “swan neck”.
Osteoarthrosis of the elbow occurs less commonly than other types of osteoarthrosis. It is characterised by osteophyte formation at the joint margins and around the articular surface of the ulnar bone leading to restriction of joint movement.
Osteoarthrosis of the shoulder is characterized by subacromial joint involvement resulting in painful abduction of the shoulder and reduced range of motion. Arthrosis of the shoulder proper occurs less commonly. In this case the shoulder joint is not distorted.
 Some patients may develop moderate atrophy of the surrounding muscles. Abduction of muscles is usually impaired.
Osteoarthrosis of the sternoclavicular joint is a common lesion and is often associated with humeroscapular periarthritis. It is clinically characterised by swelling, deformity of a joint and pain on movement. Osteoarthrosis of the sternoclavicular joint may be related to arthritis.
Osteoarthrosis of the ankle is never primary. It is often secondary to injury. It causes reduced range of motion of a joint and restriction of motor activity resulting in lack of productivity.
Osteoarthrosis of the 1st metatarsophalangial joint occurs most frequently and is typically associated with impaired static position, such as transverse or longitudinal platypodia, injury or occupational overload. It is characterised by tenderness, restriction of movement of the big toe, difficulty in walking. Transverse platypodia causes the big toe to incline outside resulting in hallux valgus and chronic bursitis of the first toe. Subluxation and dislocation of the head of metatarsal bone occurs quite often.
Polyosteoarthrosis is characterised by multiple lesions of peripheral and intervertebral joints.
It is clinically characterised by arthrosis, diskopathy and numerous tendopathies. Joint lesions are typically bilateral and symmetric. Weight-bearing joints, such as hip, knee and distal interphalangeal joints, are commonly affected. Joints of the big toe, thumb and ankle are less commonly affected.
Degenerate-dystrophic changes of spine joints are also referred to as osteoarthrosis.
Some patients may develop moderate atrophy of the surrounding muscles. Abduction of muscles is usually impaired.
Osteoarthrosis of the sternoclavicular joint is a common lesion and is often associated with humeroscapular periarthritis. It is clinically characterised by swelling, deformity of a joint and pain on movement. Osteoarthrosis of the sternoclavicular joint may be related to arthritis.
Osteoarthrosis of the ankle is never primary. It is often secondary to injury. It causes reduced range of motion of a joint and restriction of motor activity resulting in lack of productivity.
Osteoarthrosis of the 1st metatarsophalangial joint occurs most frequently and is typically associated with impaired static position, such as transverse or longitudinal platypodia, injury or occupational overload. It is characterised by tenderness, restriction of movement of the big toe, difficulty in walking. Transverse platypodia causes the big toe to incline outside resulting in hallux valgus and chronic bursitis of the first toe. Subluxation and dislocation of the head of metatarsal bone occurs quite often.
Polyosteoarthrosis is characterised by multiple lesions of peripheral and intervertebral joints.
It is clinically characterised by arthrosis, diskopathy and numerous tendopathies. Joint lesions are typically bilateral and symmetric. Weight-bearing joints, such as hip, knee and distal interphalangeal joints, are commonly affected. Joints of the big toe, thumb and ankle are less commonly affected.
Degenerate-dystrophic changes of spine joints are also referred to as osteoarthrosis.
 These changes usually occur in the lumbar and cervical parts of the spine. Depending on localization, changes are manifested clinically by spastic, neurologic and vegetative disorders. Patients usually have pain and joint stiffness in different parts of the spine as well as pain syndrome which is similar to secondary radiculitis. Spasm of paravertebral muscles occurs quite often. Compression of nerve roots causes either radicular pain or paresthesia, weakening of reflexes and disorders of motor activity. Compression of the vertebral artery may cause cerebral blood flow disturbances which are clinically manifested by dizziness, headache and vision disorders (blurring, diplopia, narrowing of visual fields and scotoms).
The above mentioned neural disorders are usually periodical and paroxysmal. Neural disorders may be caused by movements of the neck or by a certain position of the neck (for example, when vertebral arteries are compressed by osteophytes). Typical features of neural disorders are pain syndrome due to compression of nerve roots and acute, sharp pain which is similar to current going through the body. The pain usually spreads downwards, aggravating during activity. It is often associated with hyperethesia or paresthesia in distal parts of the human body. In proximal parts of the body patients often have pain. Sense and movement disorders as well as changes of reflexes are observed less commonly. Movement disorders associated with weakness, hypertrophy and hypotonia may also occur. Hyporeflexia is most commonly observed on one side of the body.
Diagnosis. Osteoarthrosis can be easily diagnosed at the extensive stage.
These changes usually occur in the lumbar and cervical parts of the spine. Depending on localization, changes are manifested clinically by spastic, neurologic and vegetative disorders. Patients usually have pain and joint stiffness in different parts of the spine as well as pain syndrome which is similar to secondary radiculitis. Spasm of paravertebral muscles occurs quite often. Compression of nerve roots causes either radicular pain or paresthesia, weakening of reflexes and disorders of motor activity. Compression of the vertebral artery may cause cerebral blood flow disturbances which are clinically manifested by dizziness, headache and vision disorders (blurring, diplopia, narrowing of visual fields and scotoms).
The above mentioned neural disorders are usually periodical and paroxysmal. Neural disorders may be caused by movements of the neck or by a certain position of the neck (for example, when vertebral arteries are compressed by osteophytes). Typical features of neural disorders are pain syndrome due to compression of nerve roots and acute, sharp pain which is similar to current going through the body. The pain usually spreads downwards, aggravating during activity. It is often associated with hyperethesia or paresthesia in distal parts of the human body. In proximal parts of the body patients often have pain. Sense and movement disorders as well as changes of reflexes are observed less commonly. Movement disorders associated with weakness, hypertrophy and hypotonia may also occur. Hyporeflexia is most commonly observed on one side of the body.
Diagnosis. Osteoarthrosis can be easily diagnosed at the extensive stage.
 Clinical history and characteristic radiographic findings can help differentiate osteoarthrosis from other conditions.
Diagnostic criteria of osteoarthrosis:
Clinical history and characteristic radiographic findings can help differentiate osteoarthrosis from other conditions.
Diagnostic criteria of osteoarthrosis:
| Clinical criteria | Radiographic criteria |
| 1. Pain in joints which occurs in the evening and/or at night. 2. Pain in joints which occurs after joint use and relieved by rest. 3. Deformity of joints due to bone enlargement, including Heberden and Bouchard nodes | 1. Joint space narrowing 2.Osteosclerosis 3.Osteophytosis |

 Differentiation of Osteoarthritis from Other Diseases.
Imaging studies of the affected joint are usually conducted in the elderly who may not have any other clinical features. For making a final diagnosis we cannot rely only on imaging or laboratory findings.
A comprehensive analysis of clinical manifestations and some additional studies may be necessary for detecting the causes of pain in joints.
Osteoarthrosis must be differentiated from arthritis of various origin, such as:
1.Rheumatoid arthritis. It should be remembered that osteoarthrosis is often associated with rheumatoid arthritis.
2. Gout.
3. Ankylosing spondylitis.
4. Diffuse hyperstosis.
5. Rheumatic polyarthritis.
Treatment of Osteoarthrosis.
Treatment of osteoarthrosis must be complex and should be undertaken considering various aetiological and pathogenetic factors which can vary. Effectiveness of treatment depends on the stage of the disease. Presence or absence of reactive synovitis plays a major role in selection of treatment. The course of the disease and underlying diseases may be also relevant. The main principle of treatment of osteoarthrosis which is often not observed is its duration and systematicity.
Differentiation of Osteoarthritis from Other Diseases.
Imaging studies of the affected joint are usually conducted in the elderly who may not have any other clinical features. For making a final diagnosis we cannot rely only on imaging or laboratory findings.
A comprehensive analysis of clinical manifestations and some additional studies may be necessary for detecting the causes of pain in joints.
Osteoarthrosis must be differentiated from arthritis of various origin, such as:
1.Rheumatoid arthritis. It should be remembered that osteoarthrosis is often associated with rheumatoid arthritis.
2. Gout.
3. Ankylosing spondylitis.
4. Diffuse hyperstosis.
5. Rheumatic polyarthritis.
Treatment of Osteoarthrosis.
Treatment of osteoarthrosis must be complex and should be undertaken considering various aetiological and pathogenetic factors which can vary. Effectiveness of treatment depends on the stage of the disease. Presence or absence of reactive synovitis plays a major role in selection of treatment. The course of the disease and underlying diseases may be also relevant. The main principle of treatment of osteoarthrosis which is often not observed is its duration and systematicity.
Main principles of treatment
1. Control of disease progression. 2. Control of pain syndrome. 3. Control of inflammation. 4. Restoration of joint function. 5. Decrease of the risk of involvement of other joints. 6. Treatment of primary disease, which initiated osteoarthrosis. 7. Improvement of the standard of living. 8. Prevention of complications. Management of osteoarthrosis depends on the severity of the disease. In mild osteoarthrosis the doctor should encourage and instruct the patient to avoid aggravating stress to the affected joint and prevent further injury. Sometimes patients may be prescribed analgesics to relieve pain. In severe osteoarthrosis, especially when the hip or knee joint is involved, a complex of nonpharmacologic interventions should be considered in addition to pharmacologic therapy, including analgesics and anti-inflammatory drugs.Medical therapy.
The following symptomatic drugs of immediate action are usually used for treating OA:
Analgesics. Local administration: Capsaicin or nonsteroidal anti-inflammatory drugs (NSAIDs) are applied to the skin around the affected joints. The goals of treatment are pain alleviation. Systemic use: 1) For the reliefs of osteoarthrosis pain the analgesic Paracetamol may be administered in moderate or high doses (up to 4 g per day). In patients with highly resistant pain, the analgesic of central action – Tramadol – should be considered. The dose should be 200 – 300 mg per day. Nonsteroidal anti-inflammatory drugs are prescribed in therapeutic doses, which are sufficient for the relief of OA pain. Nonsteroidal anti-inflammatory drugs are also administered to a patient displaying signs of synovitis. When choosing the treatment, the doctor should consider the age of the patient, concomitant diseases, side effects, such as drug gastropathy, and effects of the drugs on cartilage metabolism. Nonsteroidal anti-inflammatory drugs (NSAIDs) should be used only when it is necessary. They decrease the risk of side effects, though, they do not effect the extent of pain relief. The patient taking nonsteroidal anti-inflammatory drugs must be supervised by the doctor. Corticosteroids. Oral administration of corticosteroids in treatment of osteoarthrosis is not considered. Singular intraarticular injections of glycocorticoids can help in aggravation of the disease. One injection is usually administered every 4 – 6 months. Muscle relaxants. Muscle relaxants, such as Baclofen, Mydocalm, Scutamil C and Sirdalud, may benefit patients with evidence of muscle spasm. Symptomatic drugs of delayed action (cartilage-modifying chondroprotectors) are structural analogs of proteoglycans and glucosaminoglycans activating anabolic processes in the cartilage matrix. Treatment of osteoarthrosis with disease-modifying medications is considered to be most beneficial and it is recommended to begin the treatment with these medications. Chondroitin sulphate is high-molecular polysacchride which participates in formation of the main substance of cartilage tissue. It should be given 1500 –1000 mg daily. Glycosamine sulphate is one of the components of the articular cartilage. It is produced in packages each containing 1,5 g of glycosamine sulphate. It should be given once a day. Structure-modifying effects of glycosamine sulphate have been proven recently. Alphlutop, which is an extract of 4 types of sea fish is also used for treating osteoarthrosis. 1 ml of the preparation contains 10 mg of the extract. The drug can be administered in two ways: 1) Intraarticular injections can be prescribed to improve the symptoms. Treatment should be started with single dose of 2,0 ml administered to a single joint twice a week. After 3 – 4 days the amount of injections should be increased up to 5 weekly. The treatment should be continued with intramuscular injections of Alphlutop (1, 0 ml daily for 3 weeks). 2) Treatment can be started with intramuscular injections of Alphlutop. The initial dose should be 1,0 ml daily for 3 weeks. The course of treatment can be repeated after 3 months. Paravertebral administration of Alphlutop is also available. The use of combined preparations containing glycosamine and chondroitin sulphate is now being studied. Preparations containing hyaluronic acid. In gonarthrosis intraarticular injections of the derivatives of hyaluronate are approved. They are considered as polysaccharides consisting of a long chain of disaccharides. The goal of pharmacotherapy is pain alleviation in the knee joint. Intraarticular injections of hyaluronic acid enables the doctor to delay surgery for some time. Patients are usually tolerant of these medications. Methods of pharmacological prevention of osteoarthrosis have not been developed yet. Nonpharmacologic treatment. I. General recommendations. 1. Reduction of joint stress is of great importance. You should try to observe the following recommendations:- It is not allowed to walk for a long time.
- In osteoarthrosis of the knee or hip joint it is not allowed to stand, squat or to be on your knees for a long time.
- It is not allowed to carry weight.
- It is recommended to avoid being overweight. Excess weight increases the load on the joints.
- Occupational adjustments and joint unloading in certain joints may be necessary.
- Aerobic and muscle-strengthening exercises may be also beneficial.
- Special diets and complexes of physical exercises (aerobic and muscle-strengthening) also give relief to patients.
- The following mechanical devices are usually advised in osteoarthrosis:
- Bandages or bracelets are typically applied to the knee, if ligaments are unstable.
- When the cervical part of the spine is involved, cervical collar can give pain relief to the patient.
- In lumber lordosis patients are advised to use lumber supports for pain alleviation.
- Joint unloading in certain joints (for example, knee, hip) by means of using a stick or going on crutches.
- Use of supinators.



